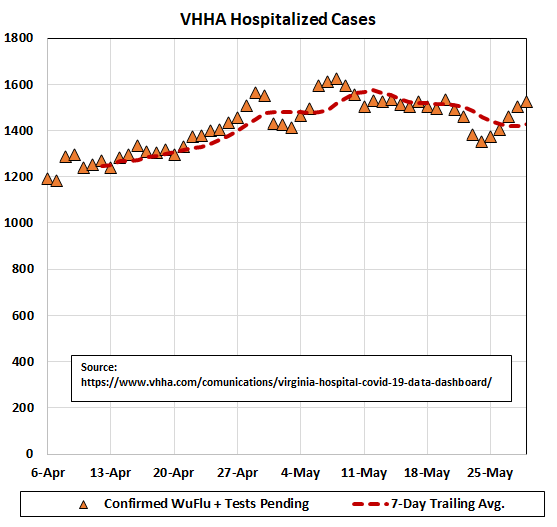
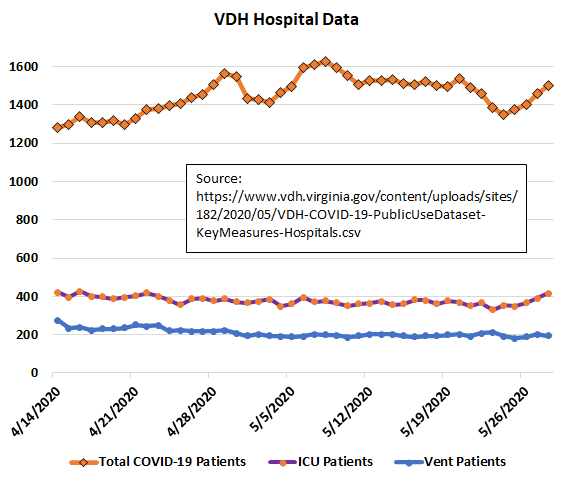
Here’s the latest from the Excel spreadsheet of John Butcher, publisher of Cranky’s blog: Daily COVID-19 hospitalizations are creeping back up, as can be seen in the graph above. And the total number of COVID-19 patients is rebounding as well as shown in the graph below:
These are not numbers anyone wants to see, least of all me, as it will reinforce Governor Ralph Northam’s predilection for maintaining his Vulcan Death Grip on Virginia’s economy. But the numbers are what they are. They’re not caused by any change in reporting protocols. They don’t reflect an increase in the number of tests. It’s a trend that bears watching.
It would be really helpful to know if the increase in hospitalizations is a generalized trend or whether it is limited to certain geographic areas or demographic groups. But that breakdown is not available on the public COVID-19 dashboards.