On Friday, the VDH reported on its COVID-19 page that 30 individuals had been identified as having contracted the coronavirus and 10 had been hospitalized. As of Saturday, VDH was stating that the number of cases had increased to 41, but it no longer provided the number of hospitalizations. The website offered no explanation for the omission. The metric is a critical one, and the public needs to know it.
As we have seen in China and Italy, hospital systems have been overwhelmed as the epidemic progresses. When hospitals run out of beds and staff to treat the afflicted, doctors go into triage mode and let some people die in order to treat those with a better chance of surviving. Virginians have every reason to wonder if a similar fate awaits the Old Dominion. Do we have enough hospital beds? Are we making the proper preparations, such as arranging for overflow facilities?
I addressed that question briefly in a blog post last week, including some numbers for hospitals in Central Virginia. This weekend, I’ve taken a more comprehensive look, and to my admittedly untutored eye the numbers look worrisome.
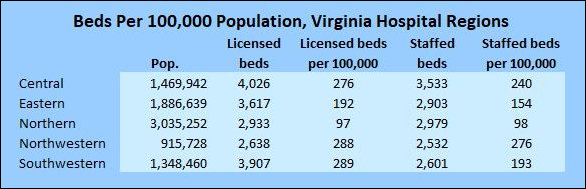
When the crunch comes, it appears that it will hit Northern Virginia the hardest. Whether you’re counting licensed beds or staffed beds, Virginia’s most populous region has the least hospital capacity of the six regions that Virginia Health Information uses to group hospitals — only 98 beds per 100,000 population.
By contrast, the best place to be is in the state’s Northwestern region, which encompasses a triangle from Charlottesville to Staunton to Winchester (as seen in the map below). That region has 276 beds per 100,000.
Measured by the number of hospital beds per 100,000 population Northern Virginia’s health system runs lean and mean. The region with three million population has roughly 3,000 licensed beds in acute-care hospitals and it staffs every last one of them. (See the green table above.) Indeed, according to VHI data, Northern Virginia hospitals somehow manage to staff a few more beds than they’re licensed for.
Running lean on the number of hospital beds helps contain health care costs, but it provides little capacity to fall back upon in the case of an epidemic. Northern Virginia has no inventory of empty beds to accommodate a flood of coronavirus patients. With 98 beds per 100,000, Northern Virginia has about one-third the number it needs to handle the epidemic load that I have postulated here.
With 154 beds per 100,000, the Eastern region has about half the number it needs.
To repeat: I have tried to make these estimates conservative. The beds-per-100,000 ratios for those two regions are low by national standards, and even lower by the standards of other industrialized nations. The average number of “curative care” beds for the U.S. as a whole was 277 per 100,000 population in 2016, according to OECD data. Thirty-one other countries had a higher proportion of curative care beds. Italy, for instance, had 317, yet its health care system has been overwhelmed. (I’m not clear what the difference is between a “curative care” bed and an “acute care” bed, so such comparisons must be made with caution.)
Needless to say, the Virginia Department of Health has much more authoritative epidemiology models and better data than I can provide here. Perhaps we can take heart that no public health official or hospital official in Virginia has expressed public concern that there might be an insufficient number of hospital beds. Indeed, Governor Ralph Northam has assured Virginians that the state has a plan in place to confront the virus. However, I have seen no hints in the public domain — announcements, press releases, news articles — that anyone is taking concrete action to handle an overflow of coronavirus patients, should it occur.
If hospitals are turning away patients for elective procedures, they are doing so without fanfare. A good modeling system should be able to predict when the epidemic will reach a critical stage — say, early April. I have not heard hospitals appeal to the public to reschedule elective procedures during that period. Meanwhile, if hospitals and public health authorities are lining up space, cots and medical equipment for pop-up facilities like those seen in China, they are doing so quietly behind the scenes. I, for one, would feel reassured to know that efforts are taking place to deal with a worst-case scenario. Such precautions would seem to be mandatory in Northern Virginia with its low ratio of hospital beds. The fact that we’re hearing nothing should make you queasy. Either we’re experiencing a failure in the plan or a failure to communicate.