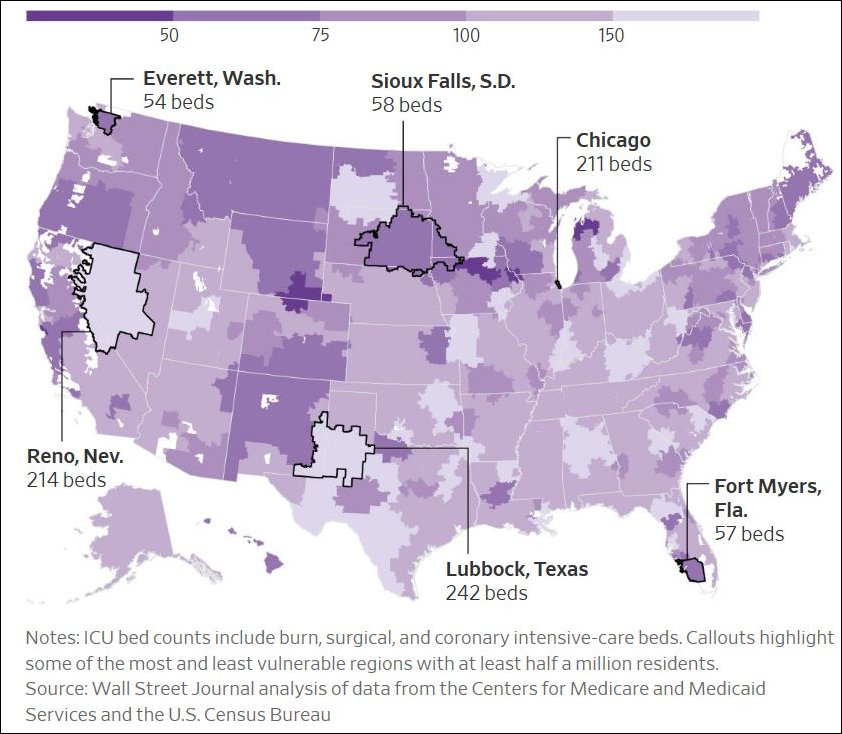
As Virginians try to formulate rational COVID-19 policy, it would be helpful to know how many ICU beds there are in Virginia hospitals. We’ve got a handle on the count of acute-care beds, but the number of ICU beds, reserved for the most critically ill patients, is perhaps an even more critical. Virginia public health authorities have not released that number, as far as I can tell, and I can’t find the data on the Internet. However, the Wall Street Journal did obtain data for ICU beds in Virginia’s hospital referral regions and published the map above showing ICU beds per 100,000 people aged 60 and older.
 Here’s a close-up of Virginia:
Here’s a close-up of Virginia:
The Washington Post breaks it down a little differently: ICU beds per 10,000 Americans aged 16 and over. The WaPo provides the following numbers for Virginia HRRs:
Arlington — 2.3
Lynchburg — 2.5
Winchester 2.5
Charlottesville — 3.2
Norfolk — 3.3
Richmond — 3.5
United States average — 3.6
Newport News — 3.6
Roanoke — 4.7