by James A. Bacon
The University of Virginia is engaging in an interesting real-world experiment in the effectiveness of COVID-19 vaccine mandates. UVa’s must-vaccinate rule for students is similar to policies at almost every other university in Virginia and many employers as well. But UVa’s COVID tracker, which is updated daily, provides a finer-grained insight into what’s happening in its community of students, faculty and staff than other dashboards I’ve viewed.
Recall that one year ago, UVa relied upon a combination of testing, masking, social distancing, online classes, and quarantining to contain the spread of the virus. Three very big changes have occurred since then. First, vaccines were introduced. Second, the super-transmissible Delta mutation became the dominant COVID-19 virus in the United States. And third, UVa reinstituted in-person classes.
This academic year, UVa went “all in” on vaccinations, requiring all students (save a handful with medical or religious exemptions) to get the jab. Students who failed to comply were “unenrolled.” Faculty and staff were “strongly urged” to take the shot. As of last week, reported UVA Today, 97% of UVa students were fully vaccinated, as was 92% of the teaching and research faculty. Additionally, everyone is required to wear masks in public indoor places. The policies and protocols are much stricter than for Virginia as a whole.
How are they working out?
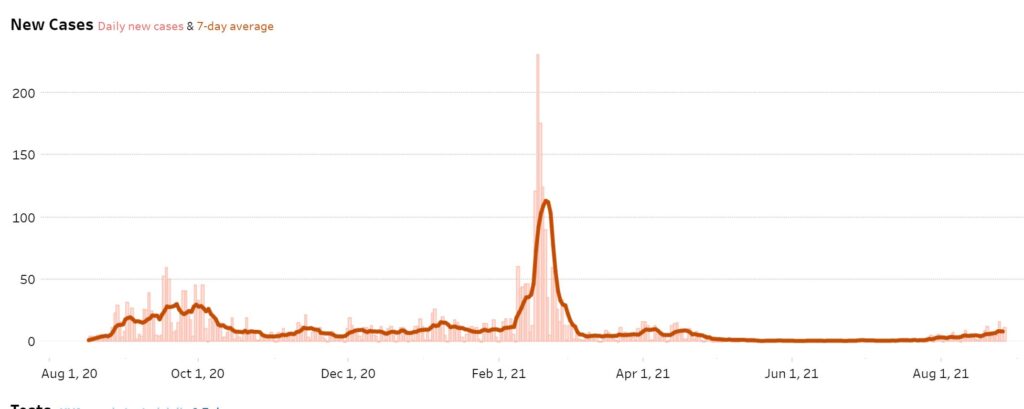
Well, a week after a return of students to classes, 80 new cases of COVID-19 have been reported. The seven-day moving average as of Aug. 26 this year was 7.6 new cases per day. That’s ahead of last year’s pace of 4.6 cases on Aug. 26.
Last year, the COVID virus spread rapidly in the days after Aug. 26, leading to a mini-spike in the seven-day moving average of 29.6 before settling back down for a few months, and then exploding in February.
I would be astonished if the pattern of spread this year matched that of last year. After all, we know that vaccines do work most of the time. Moreover, given the large number of of people who tested positive for the virus last year, many in the UVa community have acquired natural immunities.
Here’s what we don’t know: How fast vaccination immunity wears off. If potency declines and students don’t get boosters, UVa could see a resurgence. We also don’t know much about the efficacy of naturally acquired immunities.
UVa, which is a medical center after all, has the capability to do something that appears to be beyond the capacity of the Virginia Department of Health: Collect deeper, more granular data that allows us to answer questions that the VDH COVID database cannot.
In an ideal world, UVa’s data collectors would compile the following on each student, faculty member and staff person:
- Date vaccinated, and with which vaccination (Pfizer, Moderna, J&J)
- Data tested positive for COVID-19, and outcome (hospitalized, and for how long)
The purpose would be to determine how many COVID-19 cases are so-called “breakthrough” cases in which the patient has been vaccinated, and how severe the cases are. UVa then could readily determine the speed at which protection from the vaccine (and naturally acquired immunity) recedes.
Several studies have been published by credible medical institutions in Israel and the U.S. concluding that naturally acquired immunity is as effective and long-lasting as vaccine-acquired immunity. We should at least consider the possibility that COVID survivors enjoy as much protection as the vaccinated do. Current public policy (and UVa policy) assumes that only the vaccines confer meaningful protection.
Who knows — maybe a well-constructed survey would find that COVID infection + vaccine provides the most protection of all. Or maybe it will find natural immunity is superior to vaccinated immunity. We won’t know until we ask the question and construct a study. Once again, I’m struck by how little we really know. Many COVID policies are operating on auto-pilot, informed more by rigid partisan political leanings than the latest clinical findings.
COVID-19 is not going away, and we’re going to have to learn to live with it. That will require creating better information systems that allow us to answer new questions as they arise, not just this year but for the foreseeable future. UVa’s COVID Tracker is a start. The university has the potential to do more. I hope it rises to the occasion.